What Is Pain At The Heel And The Best Ways To Eliminate It

Overview
There are many diagnoses within the differential of heel pain; however, plantar fasciitis is the most common cause of heel pain for which professional care is sought. Approximately 10% of the United States population experiences bouts of heel pain, which results in 1 million visits per year to medical professionals for treatment of plantar fasciitis. The annual cost of treatments for plantar fasciitis is estimated to be between $192 and $376 million dollars. The etiology of this condition is multifactorial, and the condition can occur traumatically; however, most cases are from overuse stresses.
Causes
Plantar fasciitis can be confused with a condition called tarsal tunnel syndrome. In tarsal tunnel syndrome, an important nerve in the foot, the tibial nerve, is trapped and pinched as it passes through the tarsal tunnel, a condition analogous to carpal tunnel syndrome in the wrist. This may cause symptoms similar to the pain of a plantar fasciitis. There are also other less common problems such as nerve entrapments, stress fractures, and fat pad necrosis, all of which can cause foot pain. Finally, several rheumatologic conditions can cause heel pain. These syndromes such as Reiter's syndrome and ankylosing spondylitis can cause heel pain similar to plantar fasciitis. If your symptoms are not typical for plantar fasciitis, or if your symptoms do not resolve with treatment, your doctor will consider these possible diagnoses.
Symptoms
Symptoms of plantar fasciitis can occur suddenly or gradually. When they occur suddenly, there is usually intense heel pain on taking the first morning steps, known as first-step pain. This heel pain will often subside as you begin to walk around, but it may return in the late afternoon or evening. When symptoms occur gradually, a more long-lasting form of heel pain will cause you to shorten your stride while running or walking. You also may shift your weight toward the front of the foot, away from the heel.
Diagnosis
Physical examination is the best way to determine if you have plantar fasciitis. Your doctor examines the affected area to determine if plantar fasciitis is the cause of your pain. The doctor may also examine you while you are sitting, standing, and walking. It is important to discuss your daily routine with your doctor. An occupation in which you stand for long periods of time may cause plantar fasciitis. An X-ray may reveal a heel spur. The actual heel spur is not painful. The presence of a heel spur suggests that the plantar fascia has been pulled and stretched excessively for a long period of time, sometimes months or years. If you have plantar fasciitis, you may or may not have a heel spur. Even if your plantar fasciitis becomes less bothersome, the heel spur will remain.
Non Surgical Treatment
A doctor may prescribe anti-inflammatory medication such as ibuprofen to help reduce pain and inflammation. Electrotherapy such as ultrasound or laser may also help with symptoms. An X-ray may be taken to see if there is any bone growth or calcification, known as a heel spur but this is not necessarily a cause of pain. Deep tissue sports massage techniques can reduce the tension in and stretch the plantar fascia and the calf muscles. Extracorporeal shock wave therapy has been known to be successful and a corticosteroid injection is also an option.

Surgical Treatment
If treatment hasn't worked and you still have painful symptoms after a year, your GP may refer you to either an orthopaedic surgeon, a surgeon who specialises in surgery that involves bones, muscles and joints, a podiatric surgeon, a podiatrist who specialises in foot surgery. Surgery is sometimes recommended for professional athletes and other sportspeople whose heel pain is adversely affecting their career. Plantar release surgery. Plantar release surgery is the most widely used type of surgery for heel pain. The surgeon will cut the fascia to release it from your heel bone and reduce the tension in your plantar fascia. This should reduce any inflammation and relieve your painful symptoms. Surgery can be performed either as, open surgery, where the section of the plantar fascia is released by making a cut into your heel, endoscopic or minimal incision surgery - where a smaller incision is made and special instruments are inserted through the incision to gain access to the plantar fascia. Endoscopic or minimal incision surgery has a quicker recovery time, so you will be able to walk normally much sooner (almost immediately), compared with two to three weeks for open surgery. A disadvantage of endoscopic surgery is that it requires both a specially trained surgical team and specialised equipment, so you may have to wait longer for treatment than if you were to choose open surgery. Endoscopic surgery also carries a higher risk of damaging nearby nerves, which could result in symptoms such as numbness, tingling or some loss of movement in your foot. As with all surgery, plantar release carries the risk of causing complications such as infection, nerve damage and a worsening of your symptoms after surgery (although this is rare). You should discuss the advantages and disadvantages of both techniques with your surgical team. Extracorporeal shockwave therapy (EST) is a fairly new type of non-invasive treatment. Non-invasive means it does not involve making cuts into your body. EST involves using a device to deliver high-energy soundwaves into your heel. The soundwaves can sometimes cause pain, so a local anaesthetic may be used to numb your heel. It is claimed that EST works in two ways. It is thought to, have a "numbing" effect on the nerves that transmit pain signals to your brain, help stimulate and speed up the healing process. However, these claims have not yet been definitively proven. The National Institute for Health and Care Excellence (NICE) has issued guidance about the use of EST for treating plantar fasciitis. NICE states there are no concerns over the safety of EST, but there are uncertainties about how effective the procedure is for treating heel pain. Some studies have reported that EST is more effective than surgery and other non-surgical treatments, while other studies found the procedure to be no better than a placebo (sham treatment).
Prevention
Factors that help prevent plantar fasciitis and reduce the risk of recurrence include. Exercises to strengthen the muscles of the lower leg and ankle. Warming up before commencing physical activity. Maintaining a healthy body weight. Avoiding high heeled footwear. Using orthotic devices such as arch supports and heel raises in footwear, particularly for people with very high arches or flat feet. Daily stretches of plantar fascia and Achilles tendon.
What Exactly Causes Pain On The Heel

Overview
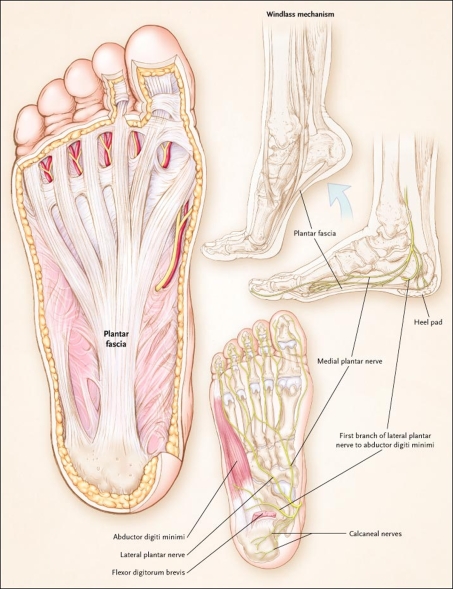
Plantar fasciosis is pain at the site of the attachment of the plantar fascia and the calcaneus (calcaneal enthesopathy), with or without accompanying pain along the medial band of the plantar fascia. Diagnosis is mainly clinical. Treatment involves calf muscle and plantar soft-tissue foot-stretching exercises, night splints, orthotics, and shoes with appropriate heel elevation. Syndromes of pain in the plantar fascia have been called plantar fasciitis; however, because there is usually no inflammation, plantar fasciosis is more correct. Other terms used include calcaneal enthesopathy pain or calcaneal spur syndrome; however, there may be no bone spurs on the calcaneus. Plantar fasciosis may involve acute or chronic stretching, tearing, and degeneration of the fascia at its attachment site.
Causes
Because the plantar fascia supports your foot and gets used every time you take a step, it has to absorb a large amount of stress and weight. If too much pressure is put on the plantar fascia, the fibers can become damaged or start to tear. The body responds by causing inflammation in the affected area. This is what causes the pain and stiffness of plantar fasciitis. Things that can increase the risk of plantar fasciitis include tight calf muscles. Tight calves make it harder to flex your foot, and this puts more stress on the plantar fascia. Weight. Carrying a few extra pounds puts added pressure on your feet every time you take a step. Activities that put a lot of stress on the feet. This includes things like running, hiking, dancing, and aerobics. Bad shoes. Footwear that doesn't give your foot the support it needs increases your risk of plantar fasciitis. You'll want to ditch any shoes that have thin soles or inadequate arch support, or ones that don't fit your feet properly. Routinely wearing high heels can also cause your Achilles tendon to contract over time, making it harder to flex your foot. Jobs that involve a lot of standing or walking on hard surfaces. Jobs that keep you on your feet all day, like waiting tables or working in a store, can cause damage to your plantar fascia. High arches, flat feet, or other foot problems. The shape of your foot can affect the way your weight is distributed on your feet when you stand. If weight distribution is a bit off, it can add to a person's risk of plantar fasciitis. How someone walks can increase the stress on certain parts of the foot too.
Symptoms
You'll typically first notice early plantar fasciitis pain under your heel or in your foot arch in the morning or after resting. Your heel pain will be worse with the first steps and improves with activity as it warms up. As plantar fasciitis deteriorates, the pain will be present more often. You can determine what stage your are in using the following guidelines. No Heel Pain, Normal! Heel pain after exercise. Heel pain before and after exercise. Heel pain before, during and after exercise. Heel pain all the time. Including at rest! This symptom progression is consistent with the four stages of a typical overuse injury. Ultimately, further trauma and delayed healing will result in the formation of calcium (bone) within the plantar fascia. When this occurs adjacent to the heel bone it is known as heel spurs, which have a longer rehabilitation period.
Diagnosis
Your doctor can usually diagnose plantar fasciitis just by talking to you and examining your feet. Rarely, tests are needed if the diagnosis is uncertain or to rule out other possible causes of heel pain. These can include X-rays of the heel or an ultrasound scan of the fascia. An ultrasound scan usually shows thickening and swelling of the fascia in plantar fasciitis.
Non Surgical Treatment
About 80% of plantar fasciitis cases resolve spontaneously by 12 months; 5% of patients end up undergoing surgery for plantar fascia release because all conservative measures have failed. For athletes in particular, the slow resolution of plantar fasciitis can be a highly frustrating problem. These individuals should be cautioned not to expect overnight resolution, especially if they have more chronic pain or if they continue their activities. . Generally, the pain resolves with conservative treatment. Although no mortality is associated with this condition, significant morbidity may occur. Patients may experience progressive plantar pain, leading to limping (antalgic gait) and restriction of activities such as walking and running. In addition, changes in weight-bearing patterns resulting from the foot pain may lead to associated secondary injury to the hip and knee joints.
Surgical Treatment
In unusual cases, surgical intervention is necessary for relief of pain. These should only be employed after non-surgical efforts have been used without relief. Generally, such surgical procedures may be completed on an outpatient basis in less than one hour, using local anesthesia or minimal sedation administrated by a trained anesthesiologist. In such cases, the surgeon may remove or release the injured and inflamed fascia, after a small incision is made in the heel. A surgical procedure may also be undertaken to remove bone spurs, sometimes as part of the same surgery addressing the damaged tissue. A cast may be used to immobilize the foot following surgery and crutches provided in order to allow greater mobility while keeping weight off the recovering foot during healing. After removal of the cast, several weeks of physical therapy can be used to speed recovery, reduce swelling and restore flexibility.
What Will Cause Plantar Fasciitis And How To Prevent It

Overview
Heel pain is most often caused by plantar fasciitis, a condition that is sometimes also called heel spur syndrome when a spur is present. Heel pain may also be due to other causes, such as a stress fracture, tendonitis, arthritis, nerve irritation, or, rarely, a cyst. Because there are several potential causes, it is important to have heel pain properly diagnosed. A foot and ankle surgeon is able to distinguish between all the possibilities and determine the underlying source of your heel pain. Plantar fasciitis is an inflammation of the band of tissue (the plantar fascia) that extends from the heel to the toes. In this condition, the fascia first becomes irritated and then inflamed, resulting in heel pain.
Causes
You are more likely to develop plantar fasciitis if you are Active, sports that place excessive stress on the heel bone and attached tissue, especially if you have tight calf muscles or a stiff ankle from a previous ankle sprain, which limits ankle movement eg. Running, ballet dancing and aerobics. Overweight. Carrying around extra weight increases the strain and stress on your plantar fascia. Pregnant. The weight gain and swelling associated with pregnancy can cause ligaments to become more relaxed, which can lead to mechanical problems and inflammation. On your feet. Having a job that requires a lot of walking or standing on hard surfaces ie factory workers, teachers and waitresses. Flat Feet or High Foot Arches. Changes in the arch of your foot changes the shock absorption ability and can stretch and strain the plantar fascia, which then has to absorb the additional force. Middle-Aged or Older. With ageing the arch of your foot may begin to sag - putting extra stress on the plantar fascia. Wearing shoes with poor support. Weak Foot Arch Muscles. Muscle fatigue allows your plantar fascia to overstress and cause injury. Arthritis. Some types of arthritis can cause inflammation in the tendons in the bottom of your foot, which may lead to plantar fasciitis. Diabetes. Although doctors don't know why, plantar fasciitis occurs more often in people with diabetes.
Symptoms
A very common complaint of plantar fasciitis is pain in the bottom of the heel. Plantar fasciitis is usually worse in the morning and may improve throughout the day. By the end of the day the pain may be replaced by a dull aching that improves with rest. Most people suffering from plantar fasciitis also complain of increased heel pain after walking for a long period of time.
Diagnosis
To arrive at a diagnosis, the foot and ankle surgeon will obtain your medical history and examine your foot. Throughout this process the surgeon rules out all the possible causes for your heel pain other than plantar fasciitis. In addition, diagnostic imaging studies such as x-rays or other imaging modalities may be used to distinguish the different types of heel pain. Sometimes heel spurs are found in patients with plantar fasciitis, but these are rarely a source of pain. When they are present, the condition may be diagnosed as plantar fasciitis/heel spur syndrome.
Non Surgical Treatment
At the first sign of soreness, massage (roll a golf ball under your foot) and apply ice (roll a frozen bottle of water under your foot). What you wear on your feet when you're not running makes a difference. Arch support is key, and walking around barefoot or in flimsy shoes can delay recovery. If pain is present for more than three weeks, see a sports podiatrist. Treatments such as orthotics, foot taping, cortisone injections, night splints, and anti-inflammatories decrease symptoms significantly in about 95 percent of sufferers within six weeks. For more stubborn cases, physical therapy may be prescribed; six months of chronic pain may benefit from shock-wave therapy, an FDA-approved plantar-fasciitis treatment.

Surgical Treatment
Most practitioners agree that treatment for plantar fasciitis is a slow process. Most cases resolve within a year. If these more conservative measures don't provide relief after this time, your doctor may suggest other treatment. In such cases, or if your heel pain is truly debilitating and interfering with normal activity, your doctor may discuss surgical options with you. The most common surgery for plantar fasciitis is called a plantar fascia release and involves releasing a portion of the plantar fascia from the heel bone. A plantar fascia release can be performed through a regular incision or as endoscopic surgery, where a tiny incision allows a miniature scope to be inserted and surgery to be performed. About one in 20 patients with plantar fasciitis will need surgery. As with any surgery, there is still some chance that you will continue to have pain afterwards.
Stretching Exercises
Calf stretch. Lean forward against a wall with one knee straight and the heel on the ground. Place the other leg in front, with the knee bent. To stretch the calf muscles and the heel cord, push your hips toward the wall in a controlled fashion. Hold the position for 10 seconds and relax. Repeat this exercise 20 times for each foot. A strong pull in the calf should be felt during the stretch. Plantar fascia stretch. This stretch is performed in the seated position. Cross your affected foot over the knee of your other leg. Grasp the toes of your painful foot and slowly pull them toward you in a controlled fashion. If it is difficult to reach your foot, wrap a towel around your big toe to help pull your toes toward you. Place your other hand along the plantar fascia. The fascia should feel like a tight band along the bottom of your foot when stretched. Hold the stretch for 10 seconds. Repeat it 20 times for each foot. This exercise is best done in the morning before standing or walking.
Work Outs For Posterior Tibial Tendon Dysfunction
Orthotics are shoe insoles, custom-made to guide the foot into corrected biomechanics. Orthotics are commonly prescribed to help with hammer toes, heel spurs, metatarsal problems, bunions, diabetic ulcerations and numerous other problems. They also help to minimize shin splints, back pain and strain on joints and ligaments. Orthotics help foot problems by ensuring proper foot mechanics and taking pressure off the parts of your foot that you are placing too much stress on. Dr. Cherine's mission is to help you realize your greatest potential and live your life to its fullest.
When the tissue of the arch of the foot becomes irritated and inflamed, even simple movements can be quite painful. Plantar fasciitis is the name that describes inflammation of the fibrous band of tissue that connects the heel to the toes. Symptoms of plantar fasciitis include pain early in the morning and pain with long walks or prolonged standing. Arch pain early in the morning is due to the plantar fascia becoming contracted and tight as you sleep through the night. Bunions develop from a weakness in the bone structure of your foot.

Do not consume food items which you are allergic to. Keep dead skin off your lips by lightly scrubbing them at least twice a week using a mild, natural ingredient such as cornflour or a lemon juice-sugar pack. I had a long road workout two weeks ago and immediately after starting having pain on the ball of my foot in this area. I have also learned buying shoes online is easy.

During the average lifetime our feet cover over 70,000 miles, the equivalent of walking four times around the world., so it's not surprising that problems can occur. Indeed around three-quarters of all adults will experience some sort of problem with their feet at some time. And without treatment most foot complaints will become gradually worse with time. This means people often endure painful conditions for far too long, and the problem can get worse. People often assume nothing can be done to help their condition, but in fact these conditions are extremely treatable. Swollen lump on big toe joint; lump may become numb but also make walking painful.
Concerning Achilles Tendonitis
 Achilles Tendonitis is an inflammation of the Achilles Tendon. This tendon attaches the muscles in the calf of the leg to the back of our heels. The Achilles Tendon is a long and thick tendon, which moves our foot down, so that the toes point to the ground (plantar flexion). This tendon can become inflamed due to the following causes. Over utilizing it, such as too much running, especially up or down hill. Trauma, such as a kick to the tendon. Shoe or boot pressure, especially at its attachment to the heel, or just above it. There are over 250,000 injuries to the Achilles Tendon annually. In fact, more Than 10% of all running injuries are to the Achilles tendon. Tendonitis may be classified as either acute or chronic. Acute Achilles Tendonitis comes on quickly, usually after a specific activity or event. It is characterized by an overstretching or tearing of some of the small fibers of the tendon, and causes pain or tenderness when walking or running. It can occur at the insertion (near the attachment to the heel bone, or further up the leg, about 4 or 5 inches above the heel. Acute tendonitis can also follow a specific injury, such as a kick to the tendon while playing soccer. Chronic Achilles Tendonitis develops gradually over time. Many times, you can feel an obvious thickening of the tendon that may be tender when squeezed, due to long standing scarring of the tendon. Pain is also present when walking or during other forms of activity, and feels better at rest.
Achilles Tendonitis is an inflammation of the Achilles Tendon. This tendon attaches the muscles in the calf of the leg to the back of our heels. The Achilles Tendon is a long and thick tendon, which moves our foot down, so that the toes point to the ground (plantar flexion). This tendon can become inflamed due to the following causes. Over utilizing it, such as too much running, especially up or down hill. Trauma, such as a kick to the tendon. Shoe or boot pressure, especially at its attachment to the heel, or just above it. There are over 250,000 injuries to the Achilles Tendon annually. In fact, more Than 10% of all running injuries are to the Achilles tendon. Tendonitis may be classified as either acute or chronic. Acute Achilles Tendonitis comes on quickly, usually after a specific activity or event. It is characterized by an overstretching or tearing of some of the small fibers of the tendon, and causes pain or tenderness when walking or running. It can occur at the insertion (near the attachment to the heel bone, or further up the leg, about 4 or 5 inches above the heel. Acute tendonitis can also follow a specific injury, such as a kick to the tendon while playing soccer. Chronic Achilles Tendonitis develops gradually over time. Many times, you can feel an obvious thickening of the tendon that may be tender when squeezed, due to long standing scarring of the tendon. Pain is also present when walking or during other forms of activity, and feels better at rest.
Causes
There are several factors that can contribute to achilles tendonitis. First, you should know that the biggest contributor to chronic achilles tendonitis is ignoring pain in your achilles tendon and running through the pain of early achilles tendonitis. If your achilles tendon is getting sore it is time to pay attention to it, immediately. Sudden increases in training can contribute to achilles tendonitis. Excessive hill running or a sudden addition of hills and speed work can also contribute to this problem. Two sole construction flaws can also aggravate achilles tendonitis. The first is a sole that is too stiff, especially at the ball of the foot. (In case you are having difficulty locating the "ball" of your foot, I mean the part where the toes join the foot and at which the foot bends) If this area is stiff than the "lever arm" of the foot is longer and the achilles tendon will be under increased tension and the calf muscles must work harder to lift the heel off the ground. The second contributing shoe design factor which may lead to continuing achilles tendon problem is excessive heel cushioning. Air filled heels, while supposedly are now more resistant to deformation and leaks are not good for a sore achilles tendon. The reason for this is quite simple. If you are wearing a shoe that is designed to give great heel shock absorption what frequently happens is that after heel contact, the heel continues to sink lower while the shoe is absorbing the shock. This further stretches the achilles tendon, at a time when the leg and body are moving forward over the foot. Change your shoes to one without this "feature". Of course another major factor is excessive tightness of the posterior leg muscles, the calf muscles and the hamstrings may contribute to prolonged achilles tendonitis. Gentle calf stretching should be performed preventatively. During a bout of acute achilles tendonitis, however, overly exuberant stretching should not be performed.
Symptoms
Symptoms vary because you can injure various areas of the muscle-tendon complex. The pain may be an acute or chronic sharp, stabbing, piercing, shooting, burning or aching. It is often most noticeable immediately after getting out of bed in the morning, or after periods of inactivity, like sitting down for lunch. After a couple minutes of walking around, it will often then settle down somewhat, before becoming symptomatic again after excessive time standing or walking. But regardless of how the pain is perceived, Achilles tendon pain should not be left untreated due to the danger that the tendon can become weak, frayed, thickened, and eventually it may rupture.
Diagnosis
There is enlargement and warmth of the tendon 1 to 4 inches above its heel insertion. Pain and sometimes a scratching feeling may be created by gently squeezing the tendon between the thumb and forefinger during ankle motion. There may be weakness in push-off strength with walking. Magnetic resonance imaging (MRI) can define the extent of degeneration, the degree to which the tendon sheath is involved and the presence of other problems in this area, but the diagnosis is mostly clinical.
Nonsurgical Treatment
The recommended treatment for Achilles tendinitis consists of icing, gentle stretching, and modifying or limiting activity. Nonsteroidal anti-inflammatory medications (NSAIDs), such as ibuprofen or naprosyn, can reduce pain and swelling. Physical therapy and the use of an orthosis (heel lift) can also be helpful. For chronic cases where tendinosis is evident and other methods of treatment have failed, surgery may be recommended to remove and repair the damaged tissue.

Surgical Treatment
Open Achilles Tendon Surgery is the traditional Achilles tendon surgery and remains the 'gold standard' of surgery treatments. During this procedure one long incision (10 to 17 cm in length) is made slightly on an angle on the back on your lower leg/heel. An angled incision like this one allows for the patient's comfort during future recovery during physical therapy and when transitioning back into normal footwear. Open surgery is performed to provide the surgeon with better visibility of the Achilles tendon. This visibility allows the surgeon to remove scar tissue on the tendon, damaged/frayed tissue and any calcium deposits or bone spurs that have formed in the ankle joint. Once this is done, the surgeon will have a full unobstructed view of the tendon tear and can precisely re-align/suture the edges of the tear back together. An open incision this large also provides enough room for the surgeon to prepare a tendon transfer if it's required. When repairing the tendon, non-absorbale sutures may be placed above and below the tear to make sure that the repair is as strong as possible. A small screw/anchor is used to reattach the tendon back to the heel bone if the Achilles tendon has been ruptured completely. An open procedure with precise suturing improves overall strength of your Achilles tendon during the recovery process, making it less likely to re-rupture in the future.
Prevention
Although Achilles tendinitis cannot be completely prevented, the risk of developing it can be lowered. Being aware of the possible causes does help, but the risk can be greatly reduced by taking the following precautions. Getting a variety of exercise - alternating between high-impact exercises (e.g. running) and low-impact exercise (e.g. swimming) can help, as it means there are days when the Achilles tendon is under less tension. Limit certain exercises - doing too much hill running, for example, can put excessive strain on the Achilles tendon. Wearing the correct shoes and replacing them when worn - making sure they support the arch and protect the heel will create less tension in the tendon. Using arch supports inside the shoe, if the shoe is in good condition but doesn't provide the required arch support this is a cheaper (and possibly more effective) alternative to replacing the shoe completely. Stretching, doing this before and after exercising helps to keep the Achilles tendon flexible, which means less chance of tendinitis developing. There is no harm in stretching every day (even on days of rest), as this will only further improve flexibility. Gradually increasing the intensity of a workout - Achilles tendinitis can occur when the tendon is suddenly put under too much strain, warming up and increasing the level of activity gradually gives your muscles time to loosen up and puts less pressure on the tendon.
MedlinePlus Medical Encyclopedia
I hit the hard streets of Chicago running. They were literally hard. I was literally running. The mountain community that had been my running grounds until that point is covered with a layer of fine red clay. But Chicago’s cement sidewalks and paved streets offered no resilience. All shock, no absorption. Friends got used to my stopping often to re-tie my disintegrating tennies so as to hold my disintegrating feet together. Nighttime was dreaded. My sciatic nerves were permanently inflamed. I had no language for that. Not that I talked much anyway. No wonder alcohol and pot were welcomed discoveries. or cavus foot is one of the most common foot problems. It is a structural foot abnormality wherein the curved part of the foot arch that runs from the heel to the toe is very high. When the arched middle part, or the gap between the underside of the foot and the ground is more, the amount of pressure exerted on the instep as well as the metatarsal bones is more, and that affects the stability of the ankles in an adverse manner. It also leads to poor shock absorption. I am sure you can easily see how walking with only one shoe on can cause your back to hurt. The cause of flat feet is related to the tissues and bones in your feet and lower legs In babies and toddlers, the condition is normal because it takes time for the tendons to tighten and form an arch. In rare cases, the bones in children’s feet become fused, causing pain. Supporting your feet is usually a first step in recovering from the condition. Your doctor may recommend that you wear orthotics, which are inserts that go inside your shoes to support your feet. For children, the doctor may prescribe special shoes or heel cups until their feet are fully formed. Lifestyle Changes The foot and lower leg are not the only areas where fallen arches can cause problems. When the arch collapses the rest of the body has to compensate. As a result the other joints become unbalanced and do not function properly. For example, the proper functioning of the knee depends upon the body weight being evenly distributed over the entire joint. When the knee has to compensate for a flattened arch, the outside of the knee is forced to take more of the load than the inside. Although the explanation of the problem can be somewhat complicated the solution to this problem is relatively simple. When bunion deformity becomes severe, the foot can hurt in different places and the mechanical function of the forefoot automatically gets affected. Although ill fitting foot wear is the main cause for bunion formation, it may also be caused by variety of conditions such as abnormal bone structure, neurological condition, excessive flexibility of the ligaments and flat feet. A foot doctor specializing in bunion surgery in Liverpool will choose a line of treatment based on the pathologies and may use a combination of procedures to successfully treat bunions. About the Author
The cause of flat feet is related to the tissues and bones in your feet and lower legs In babies and toddlers, the condition is normal because it takes time for the tendons to tighten and form an arch. In rare cases, the bones in children’s feet become fused, causing pain. Supporting your feet is usually a first step in recovering from the condition. Your doctor may recommend that you wear orthotics, which are inserts that go inside your shoes to support your feet. For children, the doctor may prescribe special shoes or heel cups until their feet are fully formed. Lifestyle Changes The foot and lower leg are not the only areas where fallen arches can cause problems. When the arch collapses the rest of the body has to compensate. As a result the other joints become unbalanced and do not function properly. For example, the proper functioning of the knee depends upon the body weight being evenly distributed over the entire joint. When the knee has to compensate for a flattened arch, the outside of the knee is forced to take more of the load than the inside. Although the explanation of the problem can be somewhat complicated the solution to this problem is relatively simple. When bunion deformity becomes severe, the foot can hurt in different places and the mechanical function of the forefoot automatically gets affected. Although ill fitting foot wear is the main cause for bunion formation, it may also be caused by variety of conditions such as abnormal bone structure, neurological condition, excessive flexibility of the ligaments and flat feet. A foot doctor specializing in bunion surgery in Liverpool will choose a line of treatment based on the pathologies and may use a combination of procedures to successfully treat bunions. About the Author
How To Choose The Right Golf Clubs For You
There is no shame in having crooked toes, but a person should see a podiatrist as soon as they can to address their foot issues before their only option is going under the knife. The sooner they see their podiatrist to treat their condition (painful or not) the sooner they can avoid long-term foot damage that will affect their life. Symptoms associated with advanced digital contracture deformity include painful motion, painful hyperkeratotic lesion (Thickened Skin), inability to wear regular shoes, contracted painful toe which is short. Padding placed under the toes, with a strap that is placed over the toes which helps to straighten the toes. A hammer toe or contracted toe is a deformity of the proximal interphalangeal joint of the second, third, or fourth toe causing it to be permanently bent, resembling a hammer Mallet toe is a similar condition affecting the distal interphalangeal joint. 1 2 Hammer toe and mallet toe – causes" Mayo Clinic Retrieved 2009-01-30 External links edit Upper limb Lower limb Head General terms Exercises may be helpful. You can try gentle stretching exercises if the toe is not already in a fixed position. PIcking up a towel with your toes can help stretch and straighten the small muscles in the foot. The extreme Y-Tune performance of Mizuno MX-200 Irons gives incredible forgiveness making golf shots easy to play and very effective. This is a quantum leap in game improvement design. Y-Tune technology successfully extends and expands the sweet area of the clubface out towards the toe to deliver amazing forgiveness on mis-hits. Through the use of a reengineered external power bar and inner Y-shaped cavity pad, the MX-200s are tuned for unbelievable forgiveness, great trajectory, and amazing feel. The MX-200 irons with Y-Tune Technology are unmatched in the industry for game improvement forgiveness and solid forged feel. Rubbing against shoe sides is not a healthy indication. Changing the shoes to the appropriate ones is not only the easiest option but economically the best also, for the treatment of mallet toe Doctors also advice use of inserts and stress relieving pads inside the shoes. Therefore it is always made to treat the problem by all methods other than surgery. The last resort is of course surgery. It is an irony that a major toe affliction like mallet toe is totally avoidable and is caused only by sheer negligence on the part of the person concerned to do things correctly matters relating to the foot. An overlapping or underlapping fifth toe is most commonly an issue based on cosmetic reasons. It is usually not a painful toe affliction. However, left untreated, the toe can become easily agitated (rubbing on the top of the shoe, pressure on tight tendons) and the toe can become inflamed or even begin losing sensation due to its unnatural placement. Hammertoe surgery involves straightening the toe through either an arthroplasty by removing a small piece of bone of the digit, or arthrodesis (fusing the joint) using a wire or implant. Following surgery, the patient is placed in a surgical shoe or boot and the patients has limited activity for several weeks. A doctor or trained medical professional should perform muscle reflex test. Although these tests are simple to perform, they require skilled assessment. Diagnosing potentially serious disease and damage to the brain and spinal cord, such as a stroke and multiple sclerosis, involves testing muscle reflexes in addition to a range of other tests. Tips In babies under the age of 1 to 1 1/2 years of age, the fibers in the brain and spinal cord are not yet completely covered with a protective myelin sheath that facilitates nerve messages. Hence, small children of this age will also show a positive Babinski sign; however, this is not a sign of disease. Callaway's top hybrids have a wider sole and 1 to 2 degrees more loft in its 2, 3 and 4 hybrids than TaylorMade's Rescue clubs. Callaway changed the weight distribution for its 2010 models, making the clubs more forgiving on off-center hits. Both companies rated gold in Golf Digest's 2010 rating of all hybrids, Callaway with its FT-iZ and Diablo Edge/Edge Tour, and TaylorMade with its Rescue TP, which has the same adjustable hosel as TaylorMade's drivers and fairway woods. Golf magazine's player panel called the Rescue TP among the best in its better-player hybrids class. In Golf magazine's game- improvement hybrids class, its panel preferred TaylorMade's Raylor. Wedges This is something I experienced as a sports injury in high school and it affects your big toe. It is an overuse injury that can cause pain and sometimes some bruising. This would generally only affect one of your toes. This can be quite painful and if left untreated, there is a chance that a infection may result. I have had a hammer toe for as long as I can remember, but have no idea why it occurred and it causes me no symptoms. It can cause pain for some people though. Claw toe can also cause pain. These are two different conditions because they affect different toe joints. Previously there was a mention of wrong footwear being the cause of hammertoe. So it is important to wear the right kind of shoes. These have to be worn for a few months post surgery and they should be preferably soft soled and comfortable. The doctor may also tell the patient to avoid narrow and high-heeled shoes. People with hammer toes suffer from pain and have difficulty wearing certain styles of shoes. Although the condition may be the result of arthritis or other diseases, the most common cause is poorly fitting shoes that force the toe into a bent position. Eventually, the deformity can become permanent, but there are treatments. Usually your negligence in wearing appropriate footwear is the main cause of Mallet toe However, you can easily solve this issue by adopting comfortable shoe. Don't forget to check your feet on regular basis for any symptoms of such abnormality. Seek as early as possible a professional advice if you experience any discomfort or spot any unusual bent toe Cure would be immediate and uncomplicated if this problem is tracked earlier. A hammertoe causes you discomfort when you walk. It can also cause you pain when trying to stretch or move the affected toe or those around it. Hammertoe symptoms may be mild or severe. Mild Symptoms
A doctor or trained medical professional should perform muscle reflex test. Although these tests are simple to perform, they require skilled assessment. Diagnosing potentially serious disease and damage to the brain and spinal cord, such as a stroke and multiple sclerosis, involves testing muscle reflexes in addition to a range of other tests. Tips In babies under the age of 1 to 1 1/2 years of age, the fibers in the brain and spinal cord are not yet completely covered with a protective myelin sheath that facilitates nerve messages. Hence, small children of this age will also show a positive Babinski sign; however, this is not a sign of disease. Callaway's top hybrids have a wider sole and 1 to 2 degrees more loft in its 2, 3 and 4 hybrids than TaylorMade's Rescue clubs. Callaway changed the weight distribution for its 2010 models, making the clubs more forgiving on off-center hits. Both companies rated gold in Golf Digest's 2010 rating of all hybrids, Callaway with its FT-iZ and Diablo Edge/Edge Tour, and TaylorMade with its Rescue TP, which has the same adjustable hosel as TaylorMade's drivers and fairway woods. Golf magazine's player panel called the Rescue TP among the best in its better-player hybrids class. In Golf magazine's game- improvement hybrids class, its panel preferred TaylorMade's Raylor. Wedges This is something I experienced as a sports injury in high school and it affects your big toe. It is an overuse injury that can cause pain and sometimes some bruising. This would generally only affect one of your toes. This can be quite painful and if left untreated, there is a chance that a infection may result. I have had a hammer toe for as long as I can remember, but have no idea why it occurred and it causes me no symptoms. It can cause pain for some people though. Claw toe can also cause pain. These are two different conditions because they affect different toe joints. Previously there was a mention of wrong footwear being the cause of hammertoe. So it is important to wear the right kind of shoes. These have to be worn for a few months post surgery and they should be preferably soft soled and comfortable. The doctor may also tell the patient to avoid narrow and high-heeled shoes. People with hammer toes suffer from pain and have difficulty wearing certain styles of shoes. Although the condition may be the result of arthritis or other diseases, the most common cause is poorly fitting shoes that force the toe into a bent position. Eventually, the deformity can become permanent, but there are treatments. Usually your negligence in wearing appropriate footwear is the main cause of Mallet toe However, you can easily solve this issue by adopting comfortable shoe. Don't forget to check your feet on regular basis for any symptoms of such abnormality. Seek as early as possible a professional advice if you experience any discomfort or spot any unusual bent toe Cure would be immediate and uncomplicated if this problem is tracked earlier. A hammertoe causes you discomfort when you walk. It can also cause you pain when trying to stretch or move the affected toe or those around it. Hammertoe symptoms may be mild or severe. Mild Symptoms